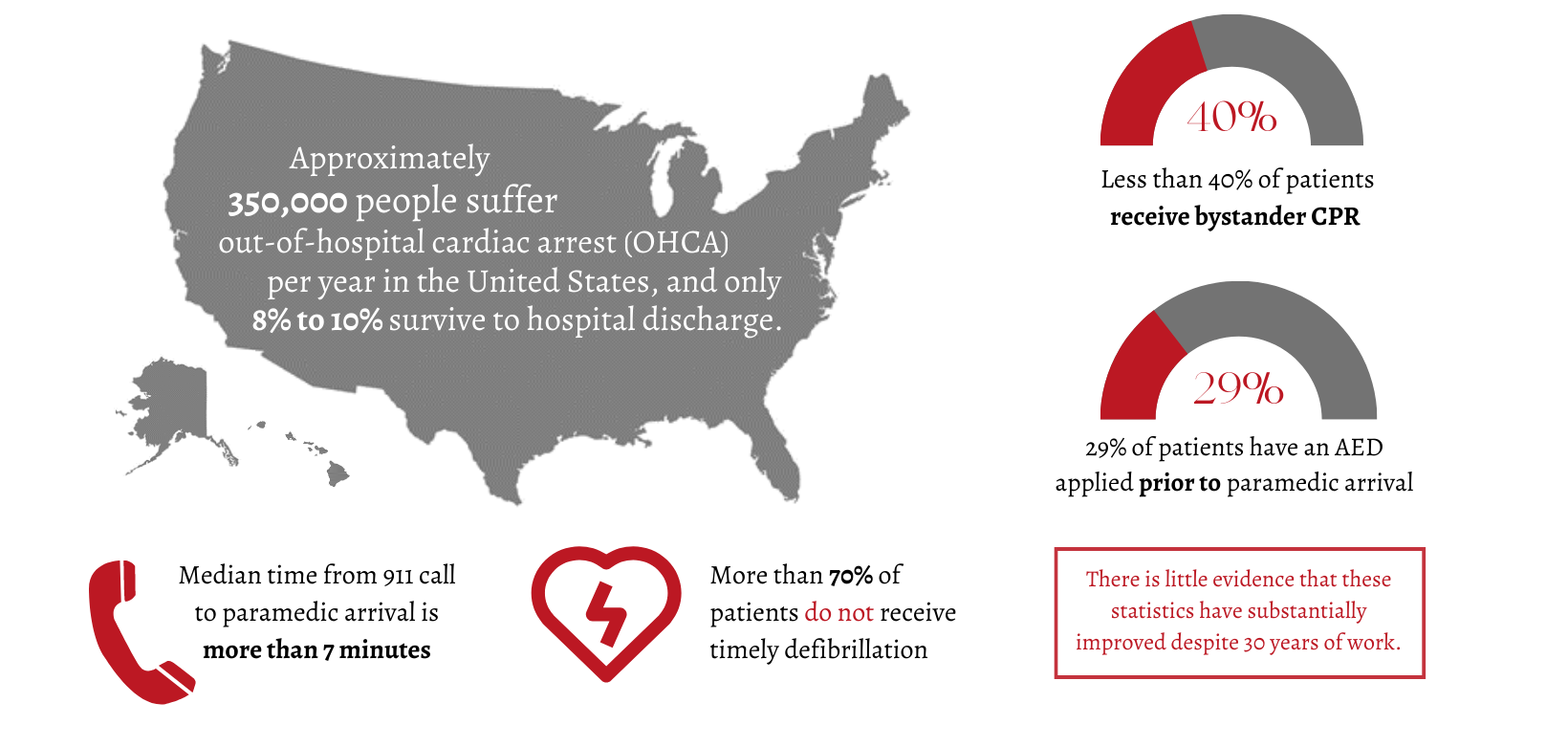
map references 1-4
The unique circumstances of OHCA (often occur at home, and only minutes separate complete recovery from irreversible brain damage) make this an extraordinarily challenging public health problem.
Like many public health problems, we believe that the critical lesion preventing progress is not the lack of knowledge about what to do but the effective systematic implementation of what we already know works.5
Thus, we believe the greatest opportunity for moving the needle on cardiac arrest outcomes, and the core intervention proposed in this clinical trial, is an intensified strategic focus centered on improved 911 recognition of OHCA, more rapid deployment of first responder defibrillation, and improved use of bystander CPR.
Out-of-hospital cardiac arrest care in the U.S. is fragmented, largely due to the lack of integration and coordination among 15,000 locally administered dispatch centers and Emergency Medical Service (EMS) agencies and over 5,200 acute care hospitals involved in treating cardiac arrest patients. This fragmentation impedes data collection for quality improvement purposes. 6-7

If successful and nationally implemented, our proposed program would translate to more than 10,000 lives saved each year.
Background
- Our group in North Carolina has worked for almost 15 years on ways to overcome this care fragmentation for acute out-of-hospital emergencies.
- The Regional Approach to Cardiovascular Emergencies (RACE) program was established in 2005 with acute myocardial infarction (MI) care.
- A coordinated statewide approach to improve the use of emergency cardiovascular care known to be effective.
- Focused on overcoming systematic barriers impeding timely and effective care.
- In 2010, as part of the Heart Rescue project, RACE was extended to patients with OHCA. Building on our systems of care and implementation experience, RACE pilot tested the implementation of key OHCA interventions subsequently highlighted in a 2015 Institute of Medicine (IOM) report, “Strategies to Improve Cardiac Arrest Survival: A Time to Act”.
- In 11 counties with complete case capture, RACE OHCA pilot observed a 25% increase in bystander CPR and first responder defibrillation and a 37% increase in survival with good neurologic function.
- Despite this, NC statewide data continues to demonstrate substantial variability in processes of care and outcomes for OHCA.
- For example, in 2017 even among these same 11 counties, bystander CPR ranged from 22% to 50%, bystander AED use ranged from 1% to 9%, first responder AED use ranged from 2% to 67%, and dispatcher recognition of OHCA ranged from 17% to 92%.
- This variability highlights the need to develop and test interventions on multiple levels that can provide consistently high-level performance and improve outcomes.
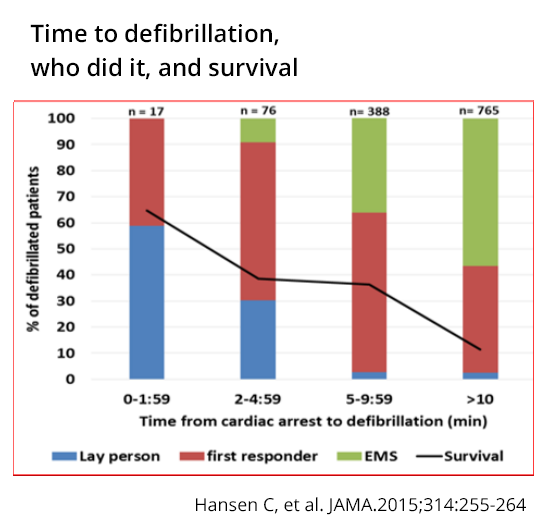
- We found that the combination of early bystander CPR and bystander or first responder defibrillation was associated with a 2- to 3-fold higher odds of patient survival with good neurologic function.
- Treatment within the first 2 minutes of cardiac arrest was particularly effective, with a 59% survival, compared with 13% for those treated after 10 minutes.8
- Earlier application of AEDs has not only resulted in the benefits of more rapid defibrillation, but also in a larger proportion of patients having a shockable rhythm.9
- While the above early intervention findings are striking, only 1.2% of our OHCA population received defibrillation in the recommended time of 2 minutes, and only 8% were defibrillated within 5 minutes.
With a systematic and comprehensive system focused on early CPR and defibrillation, our cluster- randomized trial can generate the high-level evidence needed to persuade health and community leaders to prioritize achieving a much higher community-wide level of CPR and AED use.
By customizing our approaches to the heterogeneous settings of cardiac arrest care across NC, our findings will be better suited for dissemination across similar settings in the U.S. 10-14
